On March 13, 2020, President Donald Trump issued emergency declarations for all states, tribes, territories and the District of Columbia under the Stafford Act in response to the COVID-19 pandemic. This unprecedented declaration made Federal Emergency Management Agency (FEMA) Public Assistance funding available. Congress appropriated an additional $45 billion for FEMA’s Disaster Relief Fund (referred to as Public Assistance funds).
On June 5, 2020 FEMA released the Disaster Relief Fund: Monthly Report, which included funding details through May 2020. As of May 31, nearly $10.2 billion had been obligated to support COVID-19 related expenses, leaving approximately $75 billion in the Disaster Relief Fund for the remainder of the 2020 fiscal year.
As hospitals and health systems face financial difficulty navigating this pandemic, they should consider seeking these Public Assistance funds for costs associated with COVID-19-related expenses. Successful grant applicants can receive funding to cover 75% of the eligible expenses. Below we will discuss the scope of eligible expenses, the application process and audit considerations.
Eligibility: Who Can Apply?
Public Assistance funds are available to nonprofit organizations operating an “eligible facility” or an “eligible service,” including:
-
Hospitals
-
Outpatient facilities
-
Rehabilitation facilities
-
Long term care facilities
Each nonprofit organization must have an Internal Revenue Service (IRS) ruling letter granting its tax-exempt status under the Internal Revenue Code or have documentation from the state showing that it is non-revenue producing and operates as a nonprofit under state law.
Scope of Funding: What Can Be reimbursed?
There are two main categories of expenses incurred by hospitals and health systems due to the COVID-19 pandemic that are eligible for FEMA Public Assistance funds — protective measures and non-congregate sheltering.
Eligible Protective Measures
FEMA may reimburse eligible emergency protective measures taken to respond to an emergency at the direction or guidance of public health officials. FEMA and the U.S. Department of Health and Human Services (HHS) will coordinate final reimbursement to ensure that federal agencies, including the HHS and the Centers for Disease Control and Prevention (CDC), do not provide duplicate assistance.
As announced by FEMA on March 19, 2020, the emergency protective measures that may be eligible for assistance include, but are not limited to:
-
Management, control and reduction of immediate threats to public health and safety:
-
Emergency Operation Center costs
-
Training specific to the declared event
-
Disinfection of eligible public facilities
-
Technical assistance to state, tribal, territorial or local governments on emergency management and control of immediate threats to public health and safety
-
-
Emergency medical care:
-
Non‐deferrable medical treatment of infected persons in a shelter or temporary medical facility
-
Related medical facility services and supplies
-
Temporary medical facilities and/or enhanced medical/hospital capacity (for treatment when existing facilities are reasonably forecasted to become overloaded in the near term and cannot accommodate the patient load or to quarantine potentially infected persons)
-
Use of specialized medical equipment
-
Medical waste disposal
-
Emergency medical transport
-
-
Medical sheltering (e.g. when existing facilities are reasonably forecasted to become overloaded in the near future and cannot accommodate needs)
-
All sheltering must be conducted in accordance with standards and/or guidance approved by HHS/CDC and must be implemented in a manner that incorporates social distancing measures
-
Non‐congregate medical sheltering is subject to prior approval by FEMA and is limited to that which is reasonable and necessary to address the public health needs of the event, is pursuant to the direction of appropriate public health officials and does not extend beyond the duration of the Public Health Emergency
-
-
Household pet sheltering and containment actions related to household pets in accordance with CDC guidelines
-
Purchase and distribution of food, water, ice, medicine and other consumable supplies, to include personal protective equipment and hazardous material suits movement of supplies and persons
-
Security and law enforcement
-
Communications of general health and safety information to the public
-
Search and rescue to locate and recover members of the population requiring assistance
-
Reimbursement for state, tribe, territory and/or local government force account overtime costs
Eligible Non-Congregate Sheltering
FEMA has also recognized that establishing non-congregate shelteringmay be necessary during the COVID-19 pandemic and may reimburse these costs. FEMA’s Regional Administrators have been delegated authority to approve requests for non-congregate sheltering for the duration of the COVID-19 pandemic. Before establishing non-congregate sheltering, the following considerations should be taken into account:
-
The non-congregate sheltering must be at the direction of and documented through an official order signed by a state, local, tribal or territorial public health official.
-
Any approval is limited to that which is reasonable and necessary to address the public health needs of the event and should not extend beyond the duration of the Public Health Emergency.
-
Applicants must follow FEMA’s Procurement Under Grants Conducted Under Exigent or Emergency Circumstances guidance and include a termination for convenience clause in their contracts.
-
Prior to approval, the applicant must provide an analysis of the implementation options that were considered and a justification for the option selected.
-
The funding for non-congregate sheltering to meet the needs of the Public Health Emergency cannot be duplicated by another federal agency, including the HHS or CDC.
-
Applicable Environmental and Historic Preservation laws, regulations and executive orders apply and must be adhered to as a condition of assistance.
Application Process: How Do We Start?
FEMA announced a simplified application process for Public Assistance funding on March 23, 2020. The agency has posted multiple related guidance documents, the most important of which is “Submitting a Public Assistance Funding Request for COVID-19: FEMA Public Assistance COVID-19 Streamlined Project Application” (Streamlined Project Application document). This document, which FEMA last updated April 10, 2020, contains three pages of details and considerations relevant to applicants before, during and after application submission. The remaining thirty pages in the document contain a copy of the actual Streamlined Project Application, which all applicants must complete online through the Public Assistance Grants Portal.
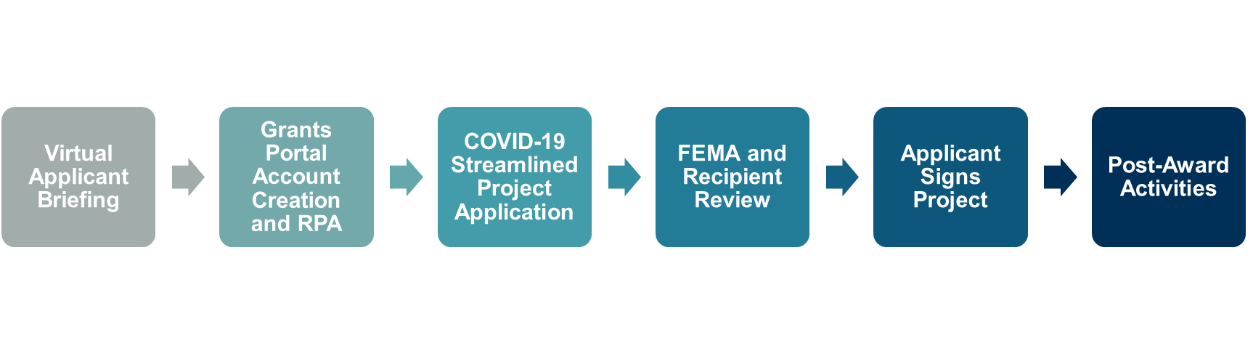
The Streamlined Project Application document should be the primary resource for applicants navigating the application process. However, as Exhibit 1 illustrates, there are steps that all applicants must take both before and after submitting the actual Streamlined Project Application.
Exhibit 1: Streamlined Application Process Steps
The first three pages of the Streamlined Project Application document cover or at least reference many pre- and post-application details. For any gaps that remain, FEMA has also published a variety of Quick Guides and a series of detailed video tutorials. Exhibit 2 contains a listing of these resources, along with a brief description of each resource.
Exhibit 2: Additional Guidance Documents
|
Guidance (with link) |
Description |
|---|---|
|
Coronavirus (COVID-19) Pandemic: Public Assistance Simplified Application |
|
|
|
|
|
|
Grants Portal Account and Request for Public Assistance: Public Assistance Applicant Quick Guide |
|
|
COVID-19 Process Overview: Public Assistance Applicant Quick Guide |
|
|
To familiarize with the FEMA staff perspective during the streamlined application process, applicants can also review the document “COVID-19 Process Overview: Public Assistance FEMA Job Aid.” The introductory language suggests that this Job Aid is intended for FEMA staff, but the Massachusetts state government posted it on the state’s COVID-19 Federal Disaster Declaration webpage.
FEMA Audit Considerations: How Do Hospitals and Health Systems Make Sure They Are Following the Rules?
FEMA carefully audits grant recipients to ensure that allocated FEMA funds were spent in accordance with federal rules. If a recipient is found to have misused funding, FEMA can de-obligate the grant and require the recipient to repay the money.
Hospital and health systems receiving FEMA funding should consider the following:
Procurement Requirements
FEMA grant recipients must adhere to certain federal procurement requirements when contracting for FEMA work. Failure to comply with the procurement requirements can lead to penalties, including de-obligation of portions of FEMA funding associated with the violation. FEMA takes procurement compliance seriously and has de-obligated portions of funds from grant recipients in the past.
As an example, a regional hospital in Ohio secured FEMA funding to help repair damage from severe storms and flooding in May and June of 2008. In 2017, after an investigation by the Office of Inspector General (OIG), FEMA de-obligated approximately $9.6 million in federal funding from Columbus Regional Hospital based on procurement violations that occurred.
Accounting and Documentation
FEMA grant recipients must account for FEMA grant funds according to federal regulations and FEMA guidelines. Generally, any expenditures must be supported by appropriate documentation specific to the project for which the funds were awarded. Organizations receiving FEMA assistance should ensure they have appropriate source documentation of all expenditures of FEMA funds and maintain a centralized expenditure tracking system.
Documentation and an active accounting system should track all expenditures of FEMA funding. OIG audits of FEMA funding identify unsupported costs, excessive charges, unrelated project costs and poor accounting as reasons for de-obligation of funds.
Prohibition of Duplication of Benefits
FEMA funds cannot duplicate assistance received from insurance claims, other assistance programs, legal awards or other benefits associated with properties or damage that is the subject of litigation. Any duplicated funds must be returned, and FEMA may adjust the reimbursement or de-obligate the duplicated funds.
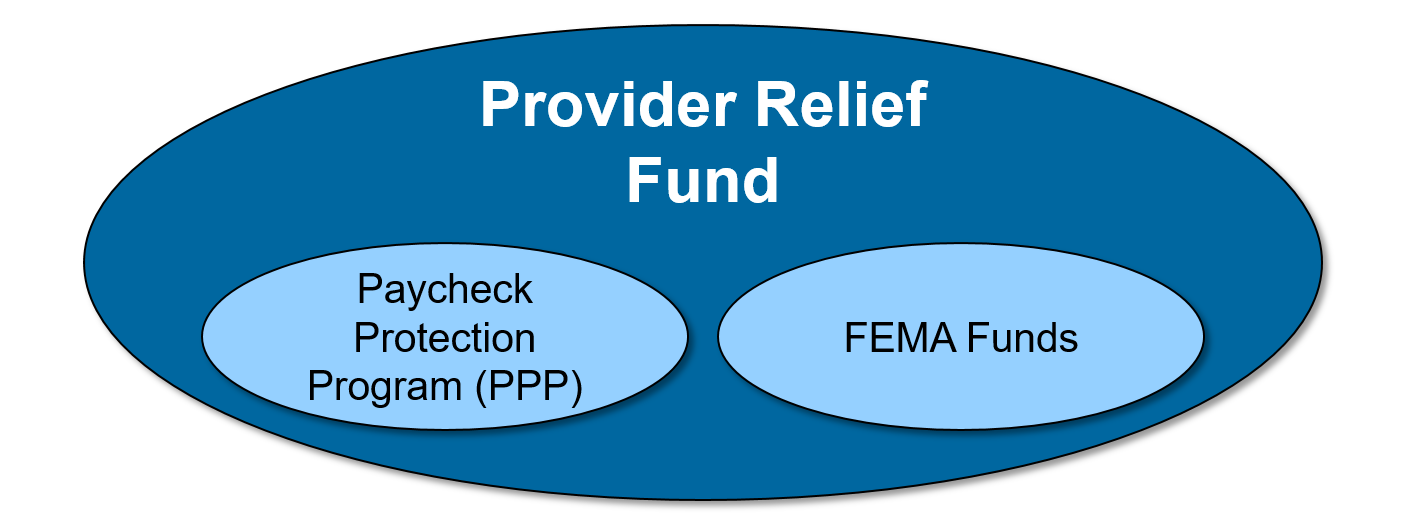
To mitigate the risk of duplicating funds, organizations should apply more specific funds to grants received for more specific programs. For example, FEMA funds are available only for certain COVID-19 related expenses, while funds from the Provider Relief Fund can be applied more broadly to offset losses related to COVID-19.
Duplication of benefits is also a common issue with insurance claims. FEMA requires grant recipients to file insurance claims to cover damage but does not require recipients to seek additional funding. Nevertheless, the recipient must report other benefits received relating to the property, including applications for other assistance, insurance proceeds or any additional compensation.
Donated funds from third parties provided for the same purpose as the FEMA funds may be applied to the non-federal cost share and are not considered a duplication of benefits if the following conditions are met:
-
The donated resource is from a third-party (a private entity or individual that is not a paid employee of the Applicant or Federal, State, Territorial or Tribal government).
-
The donated resource is necessary and reasonable for accomplishment of the project.
-
The applicant uses the resource in the performance of eligible work and within the respective project’s period of performance.
-
The applicant or volunteer organization tracks the resources and work performed, including description, specific locations and hours. Donated resources for Permanent Work (PW) must be tracked to the specific PW for which it is associated.
Failure to track and report duplicated benefits may result in de-obligation of FEMA funds. In 2009, FEMA de-obligated $1.5 million of federal funds from a California-based community health system due to a failure to report a duplication of benefits associated with FEMA funding awarded for repairs following the Northridge earthquake in January of 1994. Similarly, a hospital in California received over $8 million in FEMA funds, but failed to recover the full $50 million face amount of its insurance property and failed to equitably allocate proceeds to all insured properties. This duplication of benefits was one of four reasons FEMA cited as its rationale for de-obligating over $1.5 million of allocated funding.








 />i
/>i